- About
- Organization
- Organization Overview
- Dean’s Office
- Department of Bioengineering and Therapeutic Sciences
- Department of Clinical Pharmacy
- Department of Pharmaceutical Chemistry
- Quantitative Biosciences Institute
- Org Chart
- Research
- Education
- Patient Care
- People
- News
- Events
My COVID-19 journey
From the ski slopes of Idaho to the ICU, a pharmacist’s encounter with the health care system as a COVID-19 patient
By Marilyn Stebbins / Thu Apr 16, 2020
As we absorb the daily news of the COVID-19 pandemic, most of us—especially in California where an order to shelter in place was declared early on by Governor Gavin Newsom—have little first-hand knowledge of what it’s like to be a COVID-19 patient in the midst of the pandemic. Marilyn Stebbins, PharmD, a UC San Francisco School of Pharmacy faculty member was not so fortunate. She shares her story here.
Through February 21
Life was normal
By all accounts, life was normal for me as I planned a short ski vacation at the end of February 2020.
I’m a healthy, fit, 58-year-old woman who enjoys distance trail running, weekly circuit training, and Pilates. I’d completed a 30K trail race just before the departure date for my vacation and looked forward to a 50K race two weeks after my return home.
I’m also a health care provider—a pharmacist—and a faculty member in the Department of Clinical Pharmacy, which is in the School of Pharmacy at UC San Francisco. UCSF is a large health sciences university and academic medical center 90 miles west of where I live in Davis, California.
The days before my trip were typical. I practice at UCSF Medical Center in a virtual transitions-of-care clinic that is also a learning environment for both PharmD degree students immersed in clinical learning experiences and PharmD postdoctoral residents. We ensure that patients being discharged from the hospital have the medications they need to transition from hospital to home and know how to use them safely and effectively.
Because our clinic is a telephonic clinic, we problem-solve cases virtually from a small room on campus, working with patients, providers, insurance companies, and pharmacies. The quarters are tight.
During this period, I had no known direct exposures to patients at high risk for COVID-19. My fellow practitioners and I were alert to the COVID-19 situation in China and to the news of passengers quarantined in their cabins on, and ultimately evacuated from, a cruise ship docked in Japan due to a COVID-19 outbreak. While two patients from outside San Francisco were being treated in our hospital for COVID-19, they were doing well and planning for discharge.
UCSF had already engaged, in late January, in anticipatory emergency planning for COVID-19. And, California’s March 19 statewide shelter-in-place order was still 27 days away.
Saturday, February 22 and Sunday, February 23
Mild symptoms
As I was preparing, on February 22, for my ski trip, I had some slight cold symptoms, so I started taking zinc every two hours and elderberry syrup. My cold did not progress.

Together with her brother-in law, Norbert Chu (left), and her husband, Charlie Stebbins (right), Marilyn Stebbins, PharmD, spent three days powder skiing, dining, and lodging in Sandpoint, Idaho.
On February 23, I flew with my husband from Sacramento to San Diego, and then to Spokane, Washington. We waited 90 minutes in the Spokane airport for my brother-in-law to arrive. Together, we rented a car and drove to Sandpoint, Idaho, to our family vacation home.
Monday, February 24 and Tuesday, February 25
Fatigued but fine
From February 24 to 25, we enjoyed some great powder skiing at Schweitzer Mountain Resort, 5.5 to 6 hours each day. While I felt fatigued, it was more muscle fatigue from overuse and exertion. Throughout our stay at Sandpoint, I was in close contact with my husband and brother-in-law. We shared a house, chairlifts, great conversations, and meals.
Wednesday, February 26
Lungs begin to burn
On our final day of skiing, I commented in the afternoon to my husband and brother-in-law that, when I took a deep breath, my lungs burned a bit. I chalked it up to the cold air and altitude, and to our intense skiing. Neither my husband nor brother-in law complained of this symptom. I had no appetite that night and barely ate any of my dinner, which is definitely not like me, especially after a long day of skiing.

Marilyn Stebbins, PharmD, takes a ski break with her husband, Charlie Stebbins, at Schweitzer Mountain Resort in Sandpoint, Idaho.
Thursday, February 27
GI issues and headache present
In the early morning, we drove to Spokane International Airport to return home to the Sacramento area. On the way, I was hit with a bout of urgent diarrhea and nausea and thought I might have food poisoning. The diarrhea continued throughout the flight and into the next day. There was no associated vomiting. I had a headache but was unaware of any fever. That afternoon, I went to my local nail salon for a manicure. My manicurist always wears a mask; I did not. I was not coughing at this time.
Friday, February 28
Influenza?
When I woke on Friday morning, I still had diarrhea and now body aches and chills—but no fever. I’d developed a dry cough, and my lungs continued to burn when I took a deeper-than-normal breath.
Although I had had a flu vaccine, I knew the CDC estimate of vaccine effectiveness this year was 40 to 60 percent. I also knew that flu was prevalent this year. Based on my symptoms, I thought I might have seasonal influenza.
I called my primary care physician who asked about any travel to China or Europe, or potential contact with anyone with suspected coronavirus. I responded no to both questions, but told her I’d traveled by air in the past week. She advised me to go to the emergency department (ED) of my local community hospital in Davis and get a chest X-ray.
I really didn’t want to go. I knew the ED would be crowded, and the wait would be long. While I still didn’t have a fever, I’d developed chills and just felt sick. I asked if it wouldn’t be quicker for me to go to an urgent care clinic. She said no; she wanted me to go to ED.
After an hour of indecisiveness, I gave in.
At the ED, I was asked the same screening questions asked by my primary care physician. Travel outside the US? Contact with anyone suspected to have coronavirus? I said no again to both questions and shared my recent travel details and my symptoms. Neither the intake staff members in the ED nor the physician assistant whom I ultimately saw were wearing personal protective equipment (PPE).
I had a chest X-ray. It showed multifocal pneumonia. My vital signs were stable. ED team members commented that, looking at me and the stability of my vital signs, they wouldn’t have expected me to have such extensive pneumonia.
I was prescribed a ten-day course of amoxicillin/clavulanic acid and a five-day course of azithromycin; both medications are antibiotics. I was given a mask and told I had community-acquired bacterial pneumonia. I was told, as well, to wear my mask, stay away from people until I felt better, and make an appointment with my physician within the next week for a follow-up X-ray and possibly a CT scan, since my pneumonia was extensive.
The ED expressed a concern that seriously concerned me as well. Due to my chest X-ray result, team members said there might be something more severe underlying my pneumonia—a possible malignancy. The thought was unsettling. I explained that my symptoms—body aches, headache, diarrhea, and nausea—felt viral, so I asked for an influenza test, which I received. The result was negative.
I filled my prescriptions, went home, and took two doses of Augmentin (amoxicillin/ clavulanic acid) and one dose (double on the first day) of azithromycin. I went to bed. I felt horrible.
I sent my primary care physician a message in MyChart, and she scheduled me for a follow-up appointment on Monday, March 2 in the afternoon. She was worried about my chest X-ray results.
Saturday, February 29 and Sunday, March 1
Sicker, weaker
Over the weekend I continued to weaken, and my symptoms intensified. I became short of breath and developed a dry cough. My body continued to ache. My diarrhea continued, so I started a probiotic to help quell any antibiotic-associated diarrhea.
When I experienced shortness of breath, I coughed and became very weak and nauseated. These symptoms continued to intensify, but I still had no fever. I sounded terrible, and I felt terrible. I’d not improved with antibiotics. I was now sleeping 18 to 20 hours a day, and my husband was sleeping in a separate room.
On Sunday, I called several family members who are also health care providers. They were adamant that I go to the ED again. I told them I was seeing my primary care physician in the afternoon the next day. They reminded me that if I had a bacterial pneumonia, I should be improving with antibiotics. As a pharmacist I knew this, of course, but I wasn’t thinking clearly. I was too sick.
Monday, March 2
Hospitalized
By Monday, I still had no fever. My husband drove me to the appointment with my primary care physician who took another chest X-ray that showed the same multifocal pneumonia.
At this point, my physician was worried that my oxygen level was dropping. It was now 93 percent on room air. It had been 99 percent on room air in the ED. She advised that if I didn’t begin to feel better soon, I should go to the ED again.
We went home. I continued to cough, be short of breath, and have nausea, headache, and diarrhea.
By this time, I was completely wiped out and couldn’t function. I couldn’t climb the stairs to my bedroom without collapsing. I wasn’t eating or drinking. I’d never been this sick. I’d no idea what the ED could do for me again, but I thought if nothing else I’d get an IV and be able to hydrate.
I asked my husband to take me to the ED at the UC Davis Medical Center in Sacramento.
In terms of the COVID-19 situation, the first community-spread case of the disease in the country had been reported several days prior at UC Davis Medical Center where the patient had been transferred with severe pneumonia from a hospital in Solano County. This patient was not initially tested because she didn’t meet initial Centers for Disease Control and Prevention (CDC) guidelines for testing until she’d been at UC Davis Medical Center for several days. It was very difficult to get a COVID-19 test at that time.
I arrived at the medical center ED at about 7:30 pm and was seen very quickly. I came into the ED wearing a droplet mask—the same one I’d been wearing since being diagnosed with pneumonia at the community hospital ED on February 28.
I was asked the same screening questions. Foreign travel? Potential exposures to people positive with coronavirus? I was placed on oxygen and swabbed for influenza. Multiple blood tests were ordered: complete blood count (CBC), comprehensive metabolic panel (CMP), procalcitonin, lactic acid, blood gases, and blood cultures. A complete respiratory viral panel was ordered. I wasn’t tested for COVID-19. I was given one dose of IV ceftriaxone as well as IV azithromycin—both antibiotics—and IV fluids.
I was extremely weak and short of breath and couldn’t control my coughing, which always led to worsening nausea and a decrease in my blood oxygenation. At one point, I was hit by a bout of diarrhea. The nurse was not in my ED room, so I asked my husband to help me to the bathroom. I could barely walk. He didn’t tell me this at the time, but later he confessed that at that moment he began to think there was a chance I could die. He’d never seen me so sick, short of breath, and incapacitated. His confession was sobering, even though I heard it much later.
I finally received Dilaudid, an opioid, to calm my cough. It gave me some relief and launched me into another world. This was the last time I saw my husband while I was hospitalized.
I was moved to another area of the ED that had an isolated reverse airflow room, and an infectious diseases consult was ordered. I still had no fever, but the cough, shortness of breath, diarrhea, nausea, and headache continued and intensified.
Tuesday, March 3
CDC guidelines and me
Infectious diseases physicians, along with their medicine colleagues, interviewed me at my bedside early in the day. From my labs—low white blood count, negative procalcitonin and lactic acid—and my symptoms, they felt I had a viral, not bacterial, pneumonia. My respiratory viral panel was negative for all viruses tested, so the team agreed it was time to test me for COVID-19. I met the criteria, even without a fever, because now I was hospitalized. I continued to receive supportive care in the ED isolation room.
At 6 pm I was tested for COVID-19, and immediately everything changed. Although I remained in my isolation room, my nurse and any physicians or other health care workers who came into my room were required to wear PPE, including headgear and gowns and, at that point, respirators. They looked like bee keepers. Someone was stationed at all times outside my room to provide instructions for properly gowning up and gowning off. Very specific protocols were followed, and no visitors were allowed in my room other than necessary medical personnel.
My symptoms of shortness of breath, dry cough, nausea, headache, and diarrhea continued, and supportive care continued.
Wednesday, March 4 and Thursday, March 5
Positive outlier
At 5 pm on March 4, less than 24 hours after the COVID-19 test, my medical team told me I was COVID-19 positive. The decision had been made by infectious diseases physicians that I’d be moved from my ED isolation room to the medical intensive care unit as a precaution in case I suddenly deteriorated and needed immediate intubation. The team had been hearing and reading about seemingly stable patients with pneumonia suddenly deteriorating. I was placed again in a negative airflow room and isolated under the same precautions using full PPE gear as before.
At this point, my husband was told to quarantine for 14 days from the last time he saw me in the ED. My pulmonary symptoms remained stable and didn’t deteriorate on oxygen, but my nausea, headache, and diarrhea continued.
The infectious diseases physicians told me that a small percentage of COVID-19 patients, like me, experienced gastrointestinal symptoms, which could present before pulmonary symptoms.
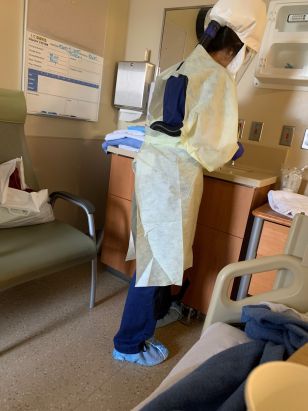
A UC Davis Medical Center ICU nurse in her PPE cares for Marilyn Stebbins, PharmD, in an isolation room.
Friday, March 6
The press release
I continued to receive supportive care, and I improved from a respiratory standpoint. I only used oxygen intermittently by March 6.
On the morning of March 6, two days after my COVID-19 positive test result was reported, I was called by a Yolo County public health nurse and asked about my case and contacts. Davis, the town in which I lived, is in Yolo County. She let me know that because I was the first reported COVID-19 positive case in the county, the county health department would be issuing a press release and would be holding a 1 pm press conference. We discussed the fact that I was not a typical hospitalized COVID-19 patient case (at that point) because of my age, fitness level, and excellent health.
Within an hour, I started receiving texts from family and friends with the press release attached. It stated that I was an “older woman with underlying health conditions.” I immediately called the county public health nurse with whom I’d spoken earlier and asked why incorrect information was released. The press release—she had since learned—was written before she talked to me. But she assured me that it would be corrected, and that the correct information would be presented at a press conference several hours later. It wasn’t.
Most people who knew I was positive were shocked to hear me described as an older woman with underlying health conditions. One of my friends said she assumed the patient was a nursing home patient, not me. Another nurse from county public health called me to apologize.
Contacts
Later in the day, the second county public health nurse asked me about my contacts, and we discussed who should be contacted and quarantined. Interestingly, the county public health department decided not to contact the nail salon even though my manicurist was in direct contact with my hands when I had symptoms. At one point, I was asked by public health if I’d call my manicurist from my hospital bed. I declined, as professional contact tracing was the responsibility of public health.
I told the public health nurse that I had close contact with my husband, and that he was already quarantined. I told her that my brother-in-law—who I explained lived in another county—was with me during our entire ski trip, had had close contact with me, and had already called his own health care provider who had put him on a 14-day quarantine. She took my brother-in-law’s phone number. I also told her that I had flown home and gave her the flight number.
I had exposed my primary care physician to the coronavirus, as well as the community hospital ED personnel during my first ED visit. While my primary care physician was quarantined by UC Davis Medical Center—her employer—county public health officers never contacted her, and it is unclear if personnel in the community hospital ED were ever contacted.
My husband is the only one who was contacted by public health. This was on March 6, and he had already been quarantined for four days.
Saturday, March 7 to Monday, March 9
Still in the ICU
I continued to have diarrhea, although the nausea was improving. My respiratory symptoms improved.
I remained in the ICU under isolation as the rules for when and how to discharge a COVID-19 patient continued to change. The decision then was to keep COVID-19 patients in the hospital until the patients demonstrated two confirmatory negative COVID-19 tests, 24 hours apart.
I was tested again the morning of March 9 and waited for the result. This test result would not come back as quickly as the first test result. I learned later in the week that all positive tests had be sent to the CDC to be confirmed.
I received physical therapy that day.
Because I was improving, and because there would likely be a delay in getting my test result, my medical team decided to send me home on Tuesday, March 10 without a negative result; they’d retest once I was home in coordination with my primary care provider. They began preparing for my transition from isolation in the hospital, to isolation at home.
The team that cared for me—the nurses, physicians, pharmacists, physical therapists, respiratory therapists, dieticians as well as the housekeeping staff—at UC Davis Medical Center was nothing short of amazing. I never felt shunned or avoided. I always felt my health and recovery were their paramount concerns. Even when my providers were shy on PPE gear, they’d call me on the phone to discuss my symptoms and talk through how I was feeling. The care they provided was truly patient-centered.
As important as the excellent medical care I received, was the virtual emotional support that just kept coming—the smiles and waves from health workers through the glass as well as the texts from family, friends, and coworkers. They meant so much to me, and I know they played a part in my recovery.
Tuesday, March 10
Uncharted territory
On March 10, I met with my UC Davis Medical Center physicians who explained they were working with county public health officials who would be responsible for my isolation and testing once I was discharged. In coordination with the medical center, public health was also responsible for determining how I’d get home.
I raised concerns about my husband’s risk. He didn’t meet CDC criteria for testing. He was still under quarantine at home. Options were discussed, including isolating him in a hotel, which didn’t seem to me to be in the public’s best interest. Plus, I wasn’t feeling strong enough to completely care for myself alone under quarantine in our two-story home. We decided, as a couple, that I’d go home but isolate ourselves in separate parts of our house.
No one could tell me if my husband would need to start his 14-day quarantine over if he were exposed to me again, or what his COVID-19 risk would be. I pushed to have him tested. If he were positive and asymptomatic, we wouldn’t have to isolate from one another, and if he were negative we’d carefully isolate from one another. He was never tested. He never developed symptoms. All we could do was simply act as if he were an asymptomatic positive case.
No one could figure out how I could get home safely and not put the public at risk. It was suggested that my husband pick me up, but again, he was under quarantine, and his COVID-19 status was unknown. It was suggested that I find a way to get my own car to the hospital and drive myself home. This was disconcerting. I’d been in the ICU for more than a week. I was still ill. I was still weak.
Nonetheless, it was a novel problem to be solved. I teach my PharmD students to identify problems and think through solutions, so this was a “do as I teach” moment from my ICU bed. Since I‘d not touched my car in weeks, I assumed it was virus free. While it’s not known for sure, studies suggest that coronaviruses may persist on surfaces for a few hours or for up to a few days.
I arranged for a willing family member to drive my car and drop it off at a deserted medical center parking lot. He then phoned me. I was masked and taken to the parking lot by a nurse in PPE and a security guard, who was masked and kept his distance, through the back exit of the medical center to avoid any contact with people. I got into the car with all of my discharge paperwork.
Once in the car, I realized that we were in completely uncharted territory. Because I was an early patient, no comprehensive evidence-based rules and systemwide policies were yet in place to address COVID-19 patients going from the hospital back into the community.
It wasn’t a comforting thought. I drove myself home.
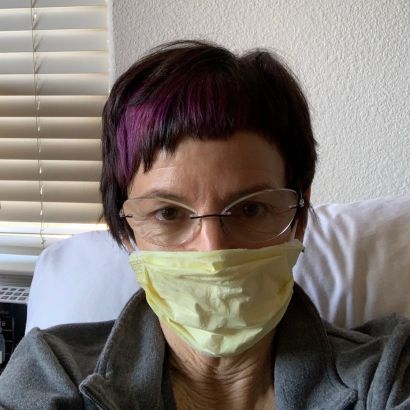
After eight days in ICU, Marilyn Stebbins, PharmD, returns home to complete her recovery from COVID-19.
Wednesday, March 11 to Thursday, April 2
Still positive
The diarrhea persisted.
The county public health department phoned me on March 13 with the news: The CDC confirmed I was still positive for the coronavirus. I was not surprised. However, during this same call they told me that my husband could come off isolation and leave the house. This was before shelter in place. This made no sense to me since I was still in the house and a known positive. He chose to remain quarantined until Monday, March 16 after being symptom-free for two-weeks from the day I was admitted to the medical center. The next day, shelter in place was started in Yolo County, so he was effectively quarantined again.
I was released from isolation at home by public health on Tuesday, March 31 because, for the first time, I’d gone 72 hours symptom-free.
My diarrhea returned on April 1 and has remained intermittent to this day. However, since I’d already been released by public health—and even though I’d not yet had a coronavirus negative test result—I was considered a recovered COVID-19 patient by public health.
My primary care physician and the infectious diseases physicians at UC Davis Medical Center agreed to test me a third time on April 2.
Friday, April 3 to present
Home alone but determined
My third test came back positive more than 36 days from my first symptoms and 31 days from my first positive test in the hospital.
I‘m waiting to be tested for a fourth time to learn if I’m still positive or if I’m negative. This will determine whether my husband and I can go back to sharing a bedroom and bathroom within our home.
Regardless of my official status as a recovered COVID-19 patient, I’ve chosen not to leave the house other than to walk my dogs on a deserted levee outside of town. Until I test negative, I won’t risk spreading the virus to others, including my untested husband.
Throughout this health episode and as a COVID-19 patient I saw the federal government downplay the COVID-19 threat. I saw a lack of readily available diagnostic testing, and no plans for patient isolation and testing after hospitalization. As an early COVID-19 patient, I experienced uncoordinated and sometimes differing guidance from the federal government and county public health departments, both of which health care providers rely on to make patient care decisions.
Once home, I felt disconnected. I wasn’t contacted by the county public health department until I’d been home for four days. On my husband’s need to quarantine, we received advice that made no sense in light of the fact that I was still positive. It would have been so much easier, and so much “healthier” for me, to have known before I came home from the hospital what my husband’s COVID-19 status was. We may not have had to have isolated from one another in the same house once I was released from ICU, and I’d not have had the constant guilt and anxiety, as a known positive, about potentially infecting him.
After I returned home, I called my manicurist to explain how bad I felt that she’d been unknowingly exposed by me. The public health department had never contacted her.
I consider myself a well-informed health care provider, and even I felt somewhat abandoned by the larger health care system—and lost—once home. It was very difficult to find answers to my questions. Thankfully, I have a very committed primary care physician who continues reply to my questions with “let me find out for you.” She has been amazing.
In many ways, I was fortunate to be an early patient. Aside from the serious lack of COVID-19 testing, I needed care at a time when there were no shortages of hospital personnel or critical shortages of equipment. I had skilled, competent, and compassionate nursing care. My physicians were top-notch and always kept me informed. I saw the ICU pharmacist every day through the glass; she was my former student. I also knew I was being cared for from afar by our UCSF pharmacist alumni and faculty who practice at UC Davis Medical Center.
I saw exceptional patient care. I also saw—having moved horizontally, over, and through the system—a deeply uncoordinated system, however unintentional. And I committed to myself to do what I can, as one pharmacist, to change the status quo.
What did I learn?
-
Patients feel a sense of abandonment in times of uncertainty. Keeping patients well-informed at all times, even when it’s only to say, “We don’t have all the answers, but we’re working on it,” is not only important, it’s our responsibility as health care providers.
-
When patients are symptomatic, navigating the health care system can be an especially overwhelming challenge. It’s our responsibility as health care providers to understand this and provide care from an empathetic as well as a clinical perspective.
-
The coordinated care of patients in and out of systems and across systems must be a priority. The provision of patient-centered care is the responsibility of health care providers. Coordinating patient-centered care is the responsibility of the larger health care infrastructure, working together and with providers.
-
Family members are a part of, not apart from, the care of patients. It’s our responsibility as health care providers to consider family members in the patient’s care plan.
What am I doing to help change the status quo?
-
I’ve donated blood for UCSF for several antibody studies and am hoping to donate my convalescent plasma as soon as I meet the criteria. I’ve also joined the UCSF COVID-19 Citizen Science Study, which is a surveillance study using an online app. I encourage each of you to do the same. Download the app or text COVID to 41411.
-
My UCSF virtual transitions-of-care team is now working with patients who’ve tested positive and negative for coronavirus and who have medication questions regarding COVID-19. It’s important to provide evidence-based answers to patients and their families; knowledge is power. It’s also important to validate their fears and frustrations with the ever-changing landscape of the COVID-19 treatment world. Fortunately, and because we practice at a health sciences university, my team is completely up-to-date on the latest science, patient care protocols, medication management protocols, and epidemiological outlook for COVID-19.
-
I’m gladly sharing my patient case with our PharmD students whose responsibility it will be, as future licensed providers, to advocate for patients; for an equitable health care system in which everyone has access to information, care, and testing when needed; and for the safety and protection of the entire health workforce.
-
Last, I’m raising my voice. Now is the time for pharmacists to step up, share the full extent of their expertise, and help identify and solve health system problems.

Marilyn Stebbins, PharmD
Pharmacists are on the front line in every community and could provide community testing when it becomes available, treatment options once these options are adequately studied, and vaccinations once developed.
Because of their access to the community, pharmacists are well positioned to help minimize the health disparities we’re seeing so clearly in this pandemic.
Pharmacists have the expertise needed to leverage emerging models of telehealth and virtual clinics to ensure that each patient has an individualized, accurate medication list and takes their medications correctly and safely. Research suggests that medical errors are the third-leading cause of death in the U.S. and that many of these deaths are directly associated with medications.
We, as pharmacists, have the opportunity and the responsibility to change the health care system into one that gives us the ability to apply the full weight of our expertise. The status quo is not acceptable, and it’s not in the best interest of our patients.
More
Watch a video (50 minutes) of Stebbins discussing her story:

Guglielmo invites faculty member Marilyn Stebbins, PharmD, to share her personal story as a COVID-19 patient. Facilitated by Grant Burningham, School editorial director.
Update: May 4, 2020
I received my eighth COVID-19 test today, May 4; the result was “no virus detected.” I need two of these negative results in a row to be considered virus free.
Update: May 6, 2020
I took my ninth confirmatory test today, May 6, and am awaiting the result. If the test is negative, I’m considered virus-free. If not, I’ll return to the two-test routine in order to get two negative tests in a row.
Update: May 7, 2020
I got my second negative. I’m now considered cleared of the virus and recovered!
It’s been 77 days since my journey with COVID-19 began. My story was one of COVID-19 in the early days when we were all learning about this threat and how to deal with it. Everyone—my providers, the public health system, my friends and family—did their best to follow existing procedures at the time. Going forward, it’s clear that we each—including me as a pharmacist and now a former COVID-19 patient—have to do our part to challenge this disease and use our expertise to prepare for whatever health threats of this magnitude we might face into the future. One of the ways pharmacists could serve the public, if authorized by California, is by ordering and administering FDA-authorized COVID-19 testing. Pharmacists are the most accessible health care providers in the community. I’m doing whatever I can to help inform decision makers about the potential of pharmacists to serve in this role.
All trademarks are held by their respective owners.
Tags
Keywords:
Category:
Sites:
School of Pharmacy, Department of Clinical Pharmacy, PharmD Degree Program
About the School: The UCSF School of Pharmacy aims to solve the most pressing health care problems and strives to ensure that each patient receives the safest, most effective treatments. Our discoveries seed the development of novel therapies, and our researchers consistently lead the nation in NIH funding. The School’s doctor of pharmacy (PharmD) degree program, with its unique emphasis on scientific thinking, prepares students to be critical thinkers and leaders in their field.




