- About
- Organization
- Organization Overview
- Dean’s Office
- Department of Bioengineering and Therapeutic Sciences
- Department of Clinical Pharmacy
- Department of Pharmaceutical Chemistry
- Quantitative Biosciences Institute
- Org Chart
- Research
- Education
- Patient Care
- People
- News
- Events
Update from the Dean - March 2017
By B. Joseph Guglielmo / Wed Mar 15, 2017

Dear UCSF School of Pharmacy Family and Friends,
As the nation debates the possibility of dramatically new directions for health care coverage, science funding, immigration, education, and more, the School is confidently moving forward, regardless of these uncertainties. We persist in working toward a time when people everywhere—all people—benefit from the School’s research, education, and patient care.
I’m proud to share this excerpt from our mission statement, which speaks volumes to the way we’ve always approached our work and will continue to do so:
We meet our mission within a culture of understanding, inclusion, equity, and respect. We recruit and support faculty members, staff members, and students who are diverse in gender, age, race, ethnicity, religion, sexual orientation, and socioeconomic status. We have a particular commitment to historically excluded populations who are currently underrepresented. We are collaborative, engaging the expertise of colleagues at UCSF and beyond to meet our mission in mutually beneficial ways.
With deep respect and an unwavering commitment to inclusion, equity, and diversity … and with my warm regards,

B. Joseph Guglielmo, PharmD
Dean
Troy C. Daniels Distinguished Professor of Pharmaceutical Sciences
UCSF School of Pharmacy
Image credit: Elisabeth Fall
Jump below to
Reducing harm
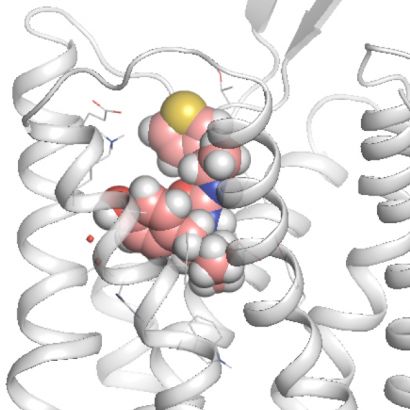
Anat Levit
PZM21, the new, potentially safer opioid drug candidate, is shown docked on the brain’s morphine receptor, the mu-opioid receptor.
Some of the most powerful outcomes of our School’s research include new ways to reduce the harm from untoward drug interactions and adverse drug events.
Drug interactions: In sub-Saharan Africa, millions of children co-infected with malaria and HIV are concomitantly treated for both infections. Francesca Aweeka, PharmD, Department of Clinical Pharmacy, led a study that revealed the World Health Organization’s preferred HIV regimen for co-infected (HIV and malaria) children over three years old significantly reduced these patients’ antimalarial blood levels. This interaction, with resultant subtherapeutic antimalarial levels, quadrupled these children’s risk for recurrent malaria.
Cancer drug toxicity: Most chemotherapy harms healthy as well as malignant cells, limiting the amount of drug that can be administered. Adam Renslo, PhD, Department of Pharmaceutical Chemistry, is targeting cancer cells based on their unusually high levels of free iron important to the cells’ proliferation. The tumor-activated cancer prodrug developed in the Renslo Lab minimizes off-target toxicity, allowing for 50-times higher doses than would normally be tolerable.
Dangerous side effects: Opioids are extremely useful in the management of pain; however, their well-known associated respiratory depression and addiction potentials limit their benefit. Brian Shoichet, PhD, also Department of Pharmaceutical Chemistry, co-led research that engineered a new opioid drug candidate, PZM21, which blocks pain as effectively as morphine, but without the associated respiratory depression and triggering of addiction.
Brian’s work was enabled by computational drug discovery technology (molecular docking) pioneered in the School. His continual efforts to advance and apply this technology earned him the 2017 Delano Award for Computational Biosciences from the American Society for Biochemistry and Molecular Biology.
QBI
A quick note here about the UCSF Quantitative Biosciences Institute (QBI) that launched last March and reports through my office. The institute uses quantitative approaches to address problems in biomedicine and biology. How does this translate for those of us who don’t speak the language of computational biology or physics? Listen and learn: “What is QBI?”
Check the QBI website and see how Director Nevan Krogan, PhD, is leading QBI, through new collaborations, workshops, and grant opportunities.
Filling new needs
Our School continues to meet the changing therapeutics needs of patients. In part, we achieve this goal through the current transformation of our doctor of pharmacy (PharmD) curriculum. We aim to prepare graduates with the critical thinking skills to meet tomorrow’s health care challenges—and also to extend the use of these skills in other fields, from business to policy.
At the same time, we are developing pharmacy practice models aimed at ensuring patients will get safe, effective, more cost-efficient care. This outcome is particularly timely as we see increasing numbers of elderly patients living with chronic medical conditions and using multiple medicines.

Marilyn Stebbins, PharmD, works with pharmacy residents and student pharmacists to ensure that patients’ medications are managed correctly.

Student pharmacist helps patient review medications to help with selection of Medicare Part D plan.
The evidence for CMM: Faculty member Marilyn Stebbins, PharmD, vice chair of clinical innovation in the Department of Clinical Pharmacy, has been collating the evidence supporting expansion of comprehensive medication management (CMM) programs. In CMM, primary care physicians make diagnoses and initiate treatment plans; collaborating pharmacists subsequently work closely with patients, optimizing their medications to meet treatment goals.
Marilyn recently co-authored a California state-issued white paper reviewing several CMM pilot programs, each suggesting improved clinical and fiscal benefits associated with this approach. In this Q&A article, she discusses her own CMM experiences and offers next steps toward wider use of the model.
Addressing affordability: Even the best personalized medication plans are useless if patients can’t afford to follow them. This year marks the 10-year anniversary of a novel PharmD student learning program, Partners in D, aimed at enabling seniors to optimize the federal Medicare Part D drug benefit. Students tackle the affordability problem head-on through the two parts of this initiative: Medicare Part D Community Outreach and a Peer Educator Program.
Our web series, starting March 13, will profile four alumni associated with this initiative. They reveal how they’re applying lessons learned from Partners in D in their widely varying careers. The program exemplifies our critical thinking approach to teaching and learning: command the facts, identify the problems, think through solutions, evaluate the results, and adjust as situations change.
Read more: Thinking it through in pharmacy school, the UCSF way
Exploring the genome
We continue to pursue a more sophisticated understanding of the human genome, consistent with the School’s vision to individualize patient therapy to maximize safety and effectiveness. Prime recent examples include:
Diabetes drug dosing: Major differences are seen among individual patients with respect to response to metformin, the key medication for type 2 diabetes. Kathy Giacomini, PhD, Department of Bioengineering and Therapeutic Sciences, and her research team discovered a genetic variation that resulted in an unexpectedly increased response to metformin—equivalent to the receipt of an extra 550 milligram dose in some people. Via inclusion of more than 2,500 patients of non-European ancestry, she determined this variant occurred far more often in African Americans.
Annotating the non-coding genome: Genes, which encode proteins, comprise just two percent of our DNA. But the rest of our genome holds myriad sequences—called regulatory elements—that control gene activity. The lab of Nadav Ahituv, PhD, Department of Bioengineering and Therapeutic Sciences, will be home to one of five new NIH-funded national centers that will define the functions and gene targets of these elements. This new knowledge, in turn, could lead to new ways to treat autism, epilepsy, heart disease, and cancer.
Epigenetics of ethnicity: Life experiences can chemically modify our DNA by attaching molecules that alter gene expression. These epigenetic changes and related health effects can be inherited. Esteban Burchard, MD, MPH, Department of Bioengineering and Therapeutic Sciences, co-led a study analyzing DNA methylation in children of Mexican or Puerto Rican ancestry (two groups who differ significantly in the rate of asthma). His study revealed hundreds of differences, a quarter of which related to cultural and environmental factors.
Foundation for the future

Ernest Prien, BS ’34, and Mary MacWilliam, EdD, UC Berkeley, 1956
Major new sources of funding are allowing us to build an ever-stronger foundation for the future. Our goal is to support and attract outstanding faculty members, pursue radically new scientific directions, and improve the way new drugs are developed and evaluated for safety and efficacy.
Endowments: Two new endowed faculty positions have been established by generous donor bequests and will be held by the chairs of the Department of Pharmaceutical Chemistry and the Department of Bioengineering and Therapeutic Sciences. We now benefit greatly from nine endowed faculty positions.
New center: A new Center for Cellular Construction, co-directed by faculty member Zev Gartner, PhD, Department of Pharmaceutical Chemistry, was established with a five-year $24 million grant from the National Science Foundation.
Grant for CERSI: The UCSF-Stanford Center of Excellence in Regulatory Science and Innovation (CERSI), co-led by Kathy Giacomini, PhD, faculty member in the Department of Bioengineering and Therapeutic Sciences, received a five-year grant of up to $25 million from the U.S. Food and Drug Administration.
Innovation rewarded: In February, five research projects—submitted by faculty and staff members and students—received funding from the Mary Anne Koda-Kimble Seed Award for Innovation. The recipients will explore “blue-sky ideas” that range from new ways to treat obesity to novel ways of accessing antibiotic-producing microbes found in soil.
UCSF PharmD in motion

Left: Grandparents Sam Kitabayashi, BSPharm ’39, and Ruriko Ando, BSPharm ’49; Right: Sharon Leaf, PharmD ’81, and student pharmacist Megan Lau, Class of 2020
This fall, our School celebrated the class of 2020’s entry into the profession with the White Coat Ceremony. Class members included students whose nations of origin ranged from Argentina to Nigeria and Uzbekistan, and included third-generation UCSF student pharmacist Megan Lau.
Megan’s family history speaks to the potential of a UCSF PharmD degree. Megan’s grandparents—Sam Kitabayashi, BSPharm ’39, and Ruriko Ando, BSPharm ’49—were experts in drug compounding and hospital pharmacy practice. Ambulatory care medication therapy management is the professional focus of Megan’s mother, Sharon Leaf, PharmD ’81. Taking a different path from her mother and grandparents, Megan’s goal is to work in drug discovery.
Read more: Three generations reflect shifts in nation, pharmacy profession
New curriculum: We continue to move ahead with the development of our new curriculum, which we’re calling the Curriculum for 2018 and Beyond. Curriculum goals are student empowerment—problem solving through critical thinking and active learning—and continual integration of increasingly complex knowledge. The new curriculum has three intertwined threads:
- The science and therapeutics thread uses organ systems (e.g., renal and cardiovascular systems) and some subspecialties (e.g., infectious diseases and oncology) as the frameworks, or blocks, for students to learn concepts of basic, clinical, and the social and administrative sciences. Faculty members will ensure the integration of these same concepts into every block. Our first block in development will center on the cardiovascular system.
- Students will explore the very latest in the therapeutic sciences and patient care, learn to effectively frame research questions, and ultimately tackle a pharmacy-related problem of personal interest. This work takes place through the curriculum’s exploration and inquiry thread.
- Through the pharmacy practice experience thread, we’ll ensure that our students experience the real-world challenges facing pharmacists, while they also provide added value to the experiential sites throughout California that host them.
With curriculum change come new needs in the areas of operations and administration, including student recruitment, student services, student housing, finance, and education technology. We also need to build staff expertise in the area of contemporary curriculum delivery, to ensure our faculty is well supported as the new curriculum evolves. We are addressing all of these now.
If this sounds like a lot, it is and should be. We’re on time and on track.
Celebrating people

E. Leong Way, PhD (center), was honored by a crowd of colleagues, friends, and family at a 100th birthday luncheon that included a look back at his distinguished research career.
We often highlight the School’s ability to achieve great things by using examples of how we are meeting the School’s mission in research, education, and patient care. However, it’s our people who are behind each success. We remain mindful of the human dimension of our enterprise, one in which one person inspires the best in others. Some notable recent examples of our best:
Frank Szoka, PhD, received the 2016 Mentor of the Year award from the American Foundation for Pharmaceutical Education (AFPE). Over the years, Frank has mentored 28 graduate students and 49 fellows.
Marcus Ferrone, PharmD, JD, and fourth-year student pharmacist Peace Chukwudi were among the honorees at the 2016 Chancellor Diversity Awards. Marcus received the Chancellor Award for Gay, Lesbian, Bisexual, and Transgender Leadership; Peace accepted the Chancellor Award for Dr. Martin Luther King, Jr. Leadership.
Since I last wrote, Edward (Eddie) Leong Way, PhD, who earned his doctorate in pharmaceutical chemistry at UCSF in 1942 and was a beloved mentor to generations of UCSF PhD and pharmacy students, celebrated his 100th birthday at our Mission Bay campus with family, friends, and colleagues.
Hall of Fame: Three of our alumni were named to the California Pharmacists Association Hall of Fame in February, at the Western Pharmacy Exchange in Palm Springs. Each was honored for their long-term distinguished service and achievement, and for being “an inspiration to the practice of pharmacy in California.” Congrats to Brian Komoto, PharmD ’81, current president of the UCSF Pharmacy Alumni Association Board of Governors; Phillip Oppenheimer, PharmD ’72; and Wilma Wong, PharmD ’73.
Not to be missed: Speaking of alumni, it’s not too late to register for Alumni Weekend 2017. We look forward to celebrating with you at the Fairmont Hotel, April 7–8. Of special note, on Saturday, April 8 the School is hosting a terrific Alumni Weekend Afternoon Program centered on the theme of collaboration and highlighting examples in the quantitative biosciences, pharmacogenomics, and education—the latter through a unique pilot with the School of Dentistry. The same night, the UCSF Pharmacy Alumni Association will hold its Gala Dinner. If you haven’t yet done so, register now.
Campus and UC updates
A transformative gift: 2017 began with the news of an unprecedented $500 million gift to the campus by the Helen Diller Foundation, which will fund endowments for faculty recruitment and retention, start-up projects for early-to mid-career scientists, scholarships for students in all of our professional degree programs, and other innovations. Given in memory of Helen, this remarkable gift is another chapter exemplifying her strong, long-term support of UCSF.
Read more: $500M gift to UCSF will support faculty, students, innovation
An enduring commitment: I began this Update with a note about the School’s mission, and I end with a note about the University of California (UC) of which we are a proud part. UC is rich in diversity, which is key to our success. When I read on the UC website that “we are here to shine a light on what’s possible,” I am reminded and assured that UC’s light shines bright because we are not afraid of differences.
I encourage you to read recent statements from the UC Office of the President regarding national decisions, and stay abreast through UC Press Room updates.
Read more:
Tags
Topics:
PharmD education, curriculum, immigration, Comprehensive medication management, malaria, HIV, targeted chemotherapy, Medicare Part D, Metformin, gene regulatory elements, Epigenetics, endowment, CERSI, Center for Cellular Construction, White Coat, AFPE, diversity, California Pharmacists Association (CPhA), gift, philanthropy
Category:
Sites:
School of Pharmacy, Department of Pharmaceutical Chemistry, Department of Bioengineering and Therapeutic Sciences, Department of Clinical Pharmacy, PharmD Degree Program, BMI, CCB, PSPG, Bioinformatics, Biophysics
About the School: The UCSF School of Pharmacy aims to solve the most pressing health care problems and strives to ensure that each patient receives the safest, most effective treatments. Our discoveries seed the development of novel therapies, and our researchers consistently lead the nation in NIH funding. The School’s doctor of pharmacy (PharmD) degree program, with its unique emphasis on scientific thinking, prepares students to be critical thinkers and leaders in their field.













